- Dry socket or alveolar osteitis is the most common complication after tooth extraction. It occurs when a blood clot fails to form or becomes dislodged.
- You can develop a dry socket if you do not follow aftercare instructions, smoke, or chew tobacco. Other common causes include bacterial contamination and trauma.
- Symptoms of a dry socket range from pain in the affected area to discomfort in the jaw and neck to mouth inflammation. Your doctor may prescribe over-the-counter pain medications to treat a dry socket.
Need professional treatment for dry socket? Use Authority Dental to find emergency dental offices in your city. It’s simple, secure and free.
Just had your tooth extracted and worried about a dry socket? Here's everything you need to know.
What causes a dry socket?
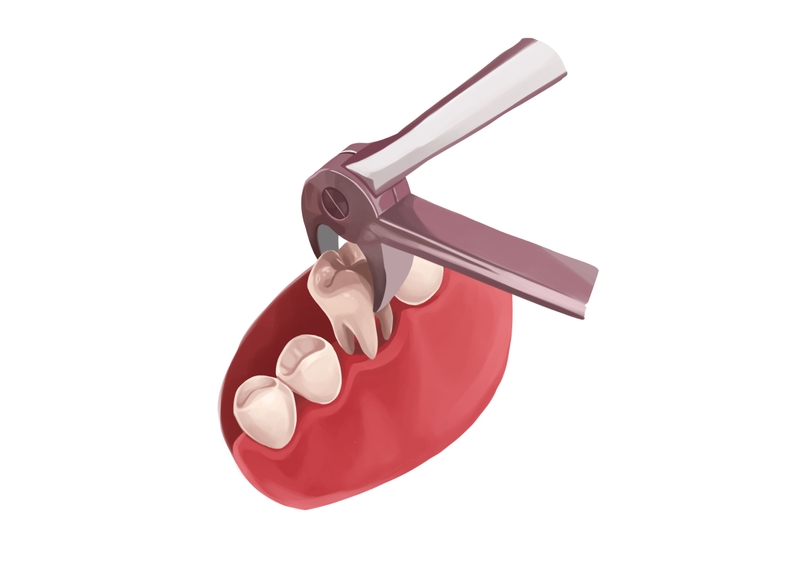
Picture by Authority Dental under CC 2.0 license
The prevalence rate of dry sockets is about 1-5% of those who recently had a tooth pulled. Interestingly, if the extraction involves lower wisdom teeth, the likelihood rises to about 38%.
Other than that, the most common dry socket causes include:
not following aftercare instructions,
smoking or chewing tobacco,
bacterial contamination, and
trauma.
Smoking and chewing tobacco are bad due to irritants and toxins. Nicotine also constricts blood vessels and decreases blood flow, which is important in healing.

Bacterial contamination may occur if you have had snacks or drinks after the blood clot was dislodged. Poor oral hygiene can also be the culprit.
Trauma happens if you poke the socket with your toothbrush or food. Sucking through straws and vigorous brushing or rinsing can also dislodge the blood clot.
The risk of getting a dry socket is increased by taking oral contraceptives, having a previous dry socket or periodontal disease, being over 25, and having a complicated extraction. Oral contraceptives introduce high levels of estrogen into the oral cavity. This may disrupt normal healing processes. This suggests that dry socket is more common in women than in men.
If you have had a dry socket before, it is likely to occur again. Let your dentist know. This might not help prevent it, but it will speed up diagnosis and treatment.
Dry socket symptoms
If you have a dry socket, pain in the affected area will be the most noticeable sign.
You may also experience the following symptoms:
significant discomfort in the jaw, neck, or ear region,
a dry opening instead of a dark clot in the extraction site,
unpleasant taste,
dullness of the jaw, and
inflammation in the mouth.
These usually appear about 3-7 days after the extraction. Dry socket signs are obvious, so it is rare for the issue to be misdiagnosed.
How to treat dry socket?
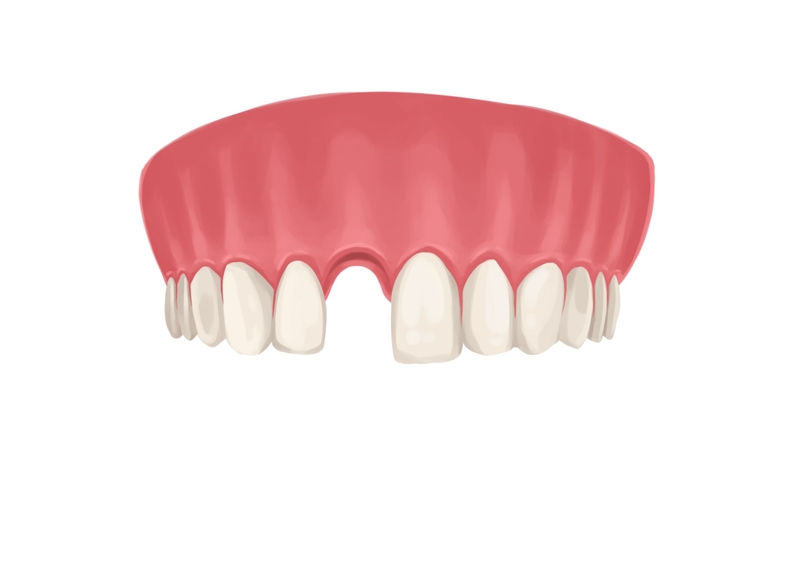
Picture by Authority Dental under CC 2.0 license
At first, start at home. Dry socket almost always heals on its own—it is all about how willing you are to experience pain.
Home remedies
If you feel pain 2-3 days after an extraction, gently rinse the area with saltwater to disinfect it. Make sure not to swish it around too vigorously, as this may worsen the problem.
Bite gently on a gauze pad or a teabag to manage the bleeding. You can also take anti-inflammatory painkillers such as ibuprofen or aspirin.
If you are still experiencing pain or swelling after 5 days, report to your dentist. OTC products may not be enough.
Professional treatment
The first step is cleaning the area to remove any food debris or bacteria. A numbing gel may be used to reduce the pain.
Your dentist will cover the extraction site with a medicated dressing or a paste. The substance that goes into the socket typically contains Eugenol (clove oil). This will stop the bleeding and prevent infection of the surgical site. He or she may also prescribe a medicated rinse or instruct you to replace the dressing at home after a few hours.
You may receive a prescription for stronger painkillers than the ones easily available at the drugstore.
How to prevent dry socket?
The most important step in preventing a dry socket is to follow post-op instructions closely. This means:
Take it easy for the rest of the day,
place a cold compress on the cheek near the removal site,
drink plenty of fluids,
do not use straws and avoid sucking motions,
Steer clear of alcohol and tobacco,
eat soft foods only, and
Rinse your mouth thoroughly for 24 hours.
Vigorous activity and exercise raise the risk of trauma and dislodging the blood clot physically. Get plenty of rest and schedule your workout for the following week.
Alcohol and tobacco can slow down healing, so stay away from those as well. Partying can lengthen the recovery period.
Eat soft foods such as puddings and yogurts to prevent trauma to the area.
Do not brush the extraction site for at least 24 hours. Try to clean the rest of your teeth without touching the area. You can use an antiseptic mouthwash to disinfect your mouth before bed. Solutions containing chlorhexidine might lower the risk of dry socket.
FAQ
How common is a dry socket?
2-5% of patients who have recently had an extraction suffer from a dry socket. It is slightly more likely in women than in men.
What does a dry socket look like?
Will dry socket heal on its own?
A dry socket often heals on its own, but you may experience a significant amount of pain. Keep the area clean by rinsing your mouth gently with warm water or saline solution, and keep gauze over the extraction site. Make sure to go easy on the area while brushing.
When can I stop worrying about the dry socket?
The chance of developing dry socket drops to 0% about 7 days after extraction.
How long does the dry socket last?
The healing time for dry socket is about 3-5 days.
How to smoke after tooth extraction without getting a dry socket?
It is best to avoid any tobacco products for at least a week after your extraction.
References
- Dry Socket Etiology, Diagnosis, and Clinical Treatment Techniques
- The effect of cigarette smoking on the severity of pain, swelling and trismus after the surgical extraction of impacted mandibular third molar
- Effect of oral contraceptive cycle on dry socket (localized alveolar osteitis)
- Dry Socket: Incidence, Clinical Features, and Predisposing Factors
- Salt water mouthwash post extraction reduced post operative complications
- Comparision Between Neocone, Alvogyl and Zinc Oxide Eugenol Packing for the Treatment of Dry Socket: A Double Blind Randomised Control Trial
- Effect of chlorhexidine rinse on the incidence of dry socket in impacted mandibular third molar extraction sites
Harry Lee, DMD
In my practice, the "day three call" is a classic scenario. A patient calls in tears because the dull ache from their extraction has suddenly turned into a throbbing pain radiating toward their ear. This is alveolar osteitis—or dry socket. I often explain to patients that it is not an infection in the traditional sense; it is a mechanical failure. The protective blood clot, which acts as a "biological band-aid," either fails to form or becomes dislodged, leaving the sensitive jawbone and nerve endings exposed to the elements.